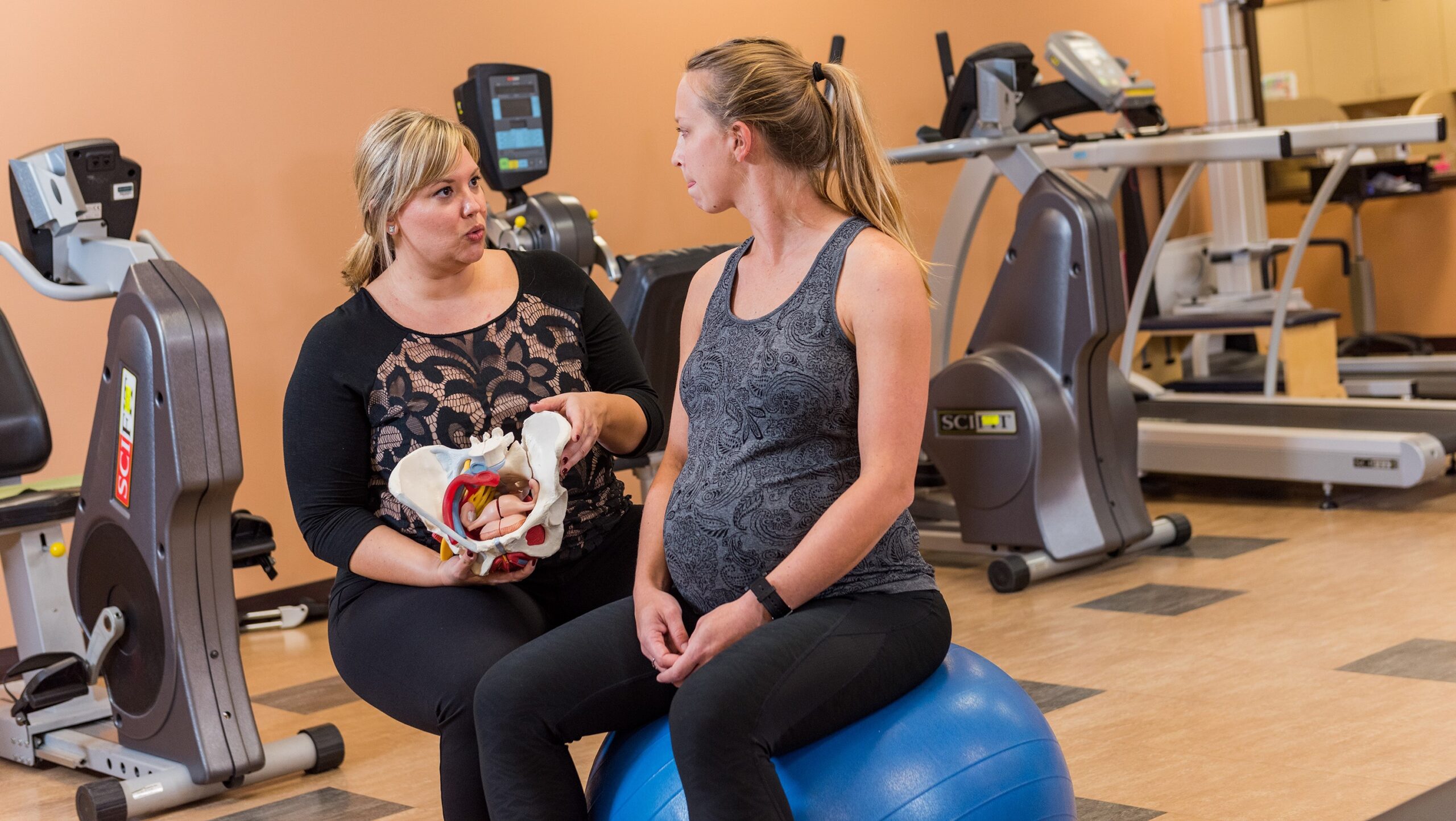Pelvic health conditions we treat
Pelvic health physical therapy is performed by therapists specially trained in treating dysfunction of the pelvic floor muscles, in both men and women. The pelvic floor is a group of muscles responsible for maintaining continence, sexual function, supporting the pelvic organs and core stability.
Bladder dysfunction
We treat urinary incontinence, urgency, frequency, nocturia/excessive night time urination, hesitancy, incomplete bladder emptying
Bowel dysfunction
Conditions we treat include fecal incontinence, anal incontinence, chronic constipation or diarrhea, fecal urgency, Irritable Bowel Syndrome (IBS) and Crohn’s disease
Pelvic pain
We provide expert therapy treatment around chronic pelvic pain, dyspareunia/pain with intercourse, pudendal neuralgia, coccydynia, pain related to endometriosis, uterine fibroids and more.
Pregnancy and postpartum
We treat conditions such as low back pain, pelvic girdle pain, gestational diabetes, diastasis rectus abdominis and more.
Oncology
Our PTs can treat issues related to breast, cervical, uterine, and ovarian cancers, prostate cancer, colorectal and anal cancers
Pelvic health services we provide
Pelvic health PTs use a variety of treatment techniques including therapeutic exercise, manual therapy, and modalities to treat dysfunction of the pelvic floor.
Therapeutic exercise
Our physical therapists provide interventions to improve motor control/coordination, strength, endurance, and power of the pelvic floor, pelvic girdle and core musculature
Manual therapy
Get hands-on techniques performed by your therapist, including but not limited to soft tissue mobilization, joint mobilizations to assist with pain relief or joint mobility and range of motion
Modalities
The most common modalities utilized in pelvic health physical therapy include electrical stimulation and surface electromyographic biofeedback.
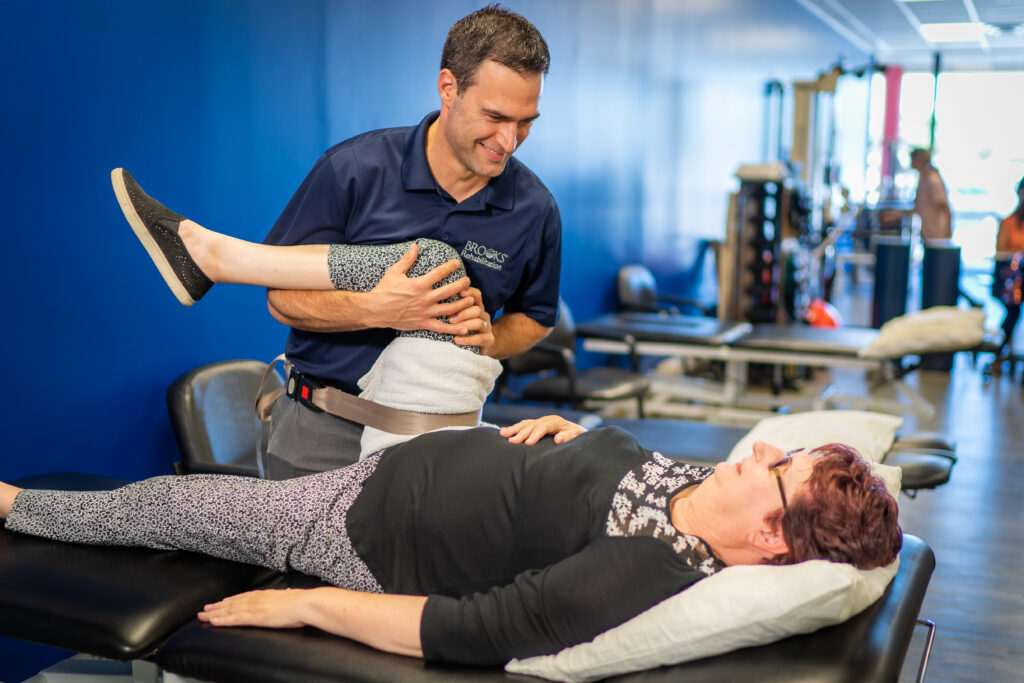
What to expect during treatment
Your plan of care with a pelvic floor physical therapist will begin with an initial evaluation in which you and your therapist will discuss your symptoms and concerns.
The pelvic health rehabilitation evaluation includes a comprehensive history and physical examination in a private room with your physical therapist. Dependent on your symptoms, examination of the pelvic girdle and pelvic floor muscles may include a direct vaginal or rectal assessment. The examination of the pelvic floor muscles is important to determine the ability of your muscles to function normally.
Your therapist’s assessment will provide insight into whether or not your muscles can contract and relax normally, if there is adequate strength and endurance, and if there are painful areas or areas of increased muscle tension. Your therapist will use findings from both the interview and the physical part of the exam to make sure you receive the proper treatment and personalized care.
Following your initial assessment, your physical therapist will develop a plan of care and work with you to establish treatment goals including a timeline for achievement of your goals. Your plan of care will be sent to your physician for review and signature.
Our pelvic health experts
Our team is made up of physical therapists with additional postgraduate training in the area of pelvic health. Pelvic health physical therapists must undergo continuing education after PT school to specialize in treating this patient population.
Request care
Brooks’ system of care accepts multiple types of insurance, as well as Medicare and Florida Medicaid. We also provide self-pay options when insurance no longer covers treatment.
Brooks partners with health care systems locally, statewide, nationally and internationally — accepting referrals from most acute hospitals and physicians.
Call (904) 875-8740 to schedule an appointment M-F, 8 a.m.-4:30 p.m., or click the button below to fill out our Request Care form.