What Women Need to Know about Their Pelvic Floor and How Physical Therapy Can Help
Back to physical health resource hub
National Women’s Health and Fitness Day is an annual celebration aiming to focus attention on the importance of regular physical activity and health awareness for all women. One area of a woman’s body that gets little attention is the Pelvic Floor. Most women know little about this area and aren’t aware of the impact that pelvic floor dysfunction can have on their health as a whole. Physical therapists specially trained in treating the pelvic floor muscles can help women to better understand this part of their body and treat dysfunctions that are often thought of as common signs of aging or childbirth.
As a physical therapist that specializes in pelvic floor rehabilitation, I am frequently asked what it is I actually do. “Are you just teaching your patients kegels?” “What should I be doing to help myself?” Let’s dive in to what pelvic floor physical therapy is and why it matters!
The pelvic floor is a group of muscles, located at the base of the pelvis that stretch from the pubic bone to the tailbone. We use our pelvic floor on a daily basis, constantly. In order to sit, stand, walk or even roll out of bed, you need your pelvis’ participation. Whether it is in transferring your body weight from one position to another, core support or maintaining continence when the timing isn’t right; the pelvic floor is almost never in a truly passive state. 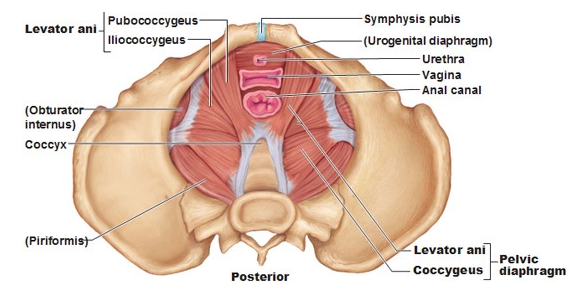 The muscle tissue of the pelvic floor has the same fiber make up as all other skeletal muscle in the body such as your biceps, quadriceps or calf muscles. This makeup gives us the ability to voluntarily control it, but also allows it to become dysfunctional. So, when this specific body region does begin to show signs of weakness, pain or dysfunction, it needs to be addressed in a similar manner as we would for a knee injury or an ankle sprain. So why is it that most individuals have never heard of this type of therapy? Do we not see dysfunction in this area as important to treat when it starts to act abnormally? It’s important to understand that some pelvic floor dysfunctions are common, but they are not normal.
The muscle tissue of the pelvic floor has the same fiber make up as all other skeletal muscle in the body such as your biceps, quadriceps or calf muscles. This makeup gives us the ability to voluntarily control it, but also allows it to become dysfunctional. So, when this specific body region does begin to show signs of weakness, pain or dysfunction, it needs to be addressed in a similar manner as we would for a knee injury or an ankle sprain. So why is it that most individuals have never heard of this type of therapy? Do we not see dysfunction in this area as important to treat when it starts to act abnormally? It’s important to understand that some pelvic floor dysfunctions are common, but they are not normal.
Rehabilitation of the pelvic floor aims to address symptoms including urinary or fecal incontinence, urinary urgency, frequency of urination, constipation, uterine/bladder/rectal prolapse, pain with intercourse, pelvic girdle pain, coccydynia (tailbone pain), changes related to pregnancy/post-partum and core weakness. Depending on the diagnosis and what is observed during the initial evaluation, a plan is developed to restore motion, strength, tissue relaxation, neural health, and/or continence. During therapy sessions, patients can expect internal or external examinations, use of biofeedback, pelvic floor strengthening or relaxation exercises, lumbar, pelvic, sacral, or coccyx spinal mobilizations to restore motion or proper alignment, and core strengthening exercises to reduce inappropriate stresses on the pelvic girdle system.
One specific exercise that I work on with patients dealing with pelvic floor weakness is a classic bridge, with a twist. Envision lying on your back with your knees bent, back flat. Now, try engaging your pelvic floor by pulling your kegel muscles up and in toward your belly button like you are trying to stop the flow of urine. Then, pull your abdominals in toward your spine and lift your hips up off the floor toward the ceiling, engaging your glutes and hamstrings. Repeat. This exercise is so effective at reducing incontinence issues and gives your whole lower body and core a good workout.
To find a pelvic floor physical therapist in your area please visit our Location page.



