Swallow This: Treat Dysphagia with Speech Pathology

Back to physical health resource hub
Did you know that speech-language pathologists (SLP) also treat swallowing disorders, which are known as dysphagia?
“I cannot tell you how many times I have sat down with a patient and the first words out of their mouth are, ‘I can talk just fine,’” said Stephanie Richardson, M.S., CCC-SLP, an SLP who works at Brooks Rehabilitation.
Most people are unaware that dysphagia is evaluated and treated by speech pathologists. In this article, we will explore:
- What is a swallowing disorder
- What causes Dysphagia
- The symptoms of swallowing disorders
- The phases of swallowing
- How patients are tested for swallowing disorders
What is Dysphagia?
Dysphagia is difficulty swallowing, which means the patient is taking more time and effort to move food or liquid from their mouth to their stomach. It becomes a concern when it is continuous and then leads to a serious medical condition.
Causes of Dysphagia
Dysphagia occurs at any age but is more common in older adults. It is usually caused by another health issue that affects the nervous system such as a stroke, head injury or dementia. It can also be caused by cancer of the mouth, gastro-oesophageal reflux disease or problems with breathing.
It can occur in children when a developmental or learning disability is present.
Symptoms of Swallowing Disorders
Here is a list of symptoms to look out for when considering if you or a loved one is experiencing dysphagia.
• Difficulty starting a swallow
• Food or liquids coming out of your nose or dribbling out of your mouth
• Excessive drooling
• Choking or coughing when eating
• Frequent throat clearing
• Trouble managing saliva leading to drooling or choking
• Painful swallowing
• Frequent respiratory infections
• Weight loss

Phases of Swallowing
Swallowing is a very complex process and a large part of overall health. If you or a loved one have any of the following symptoms, talk to your primary care physician and ask for a speech-language pathologist referral for dysphagia. There are three phases for swallowing food.
Phase One: Oral Phase
The first phase of swallowing is the oral phase. This requires your mouth to open, insert the food, contain it with your lips and then use the tongue to move the food in a circular motion while utilizing your teeth to break down the food.
During this time you must keep the food in the oral cavity of your mouth, so it does not create a gag or go down before you are ready, causing you to choke.
The tongue is essential in the swallowing process. It is made up of eight muscles intertwined together to function like an octopus tentacle and is flexible, strong and agile. Any weakness, distortion or loss of tongue can cause swallowing problems.

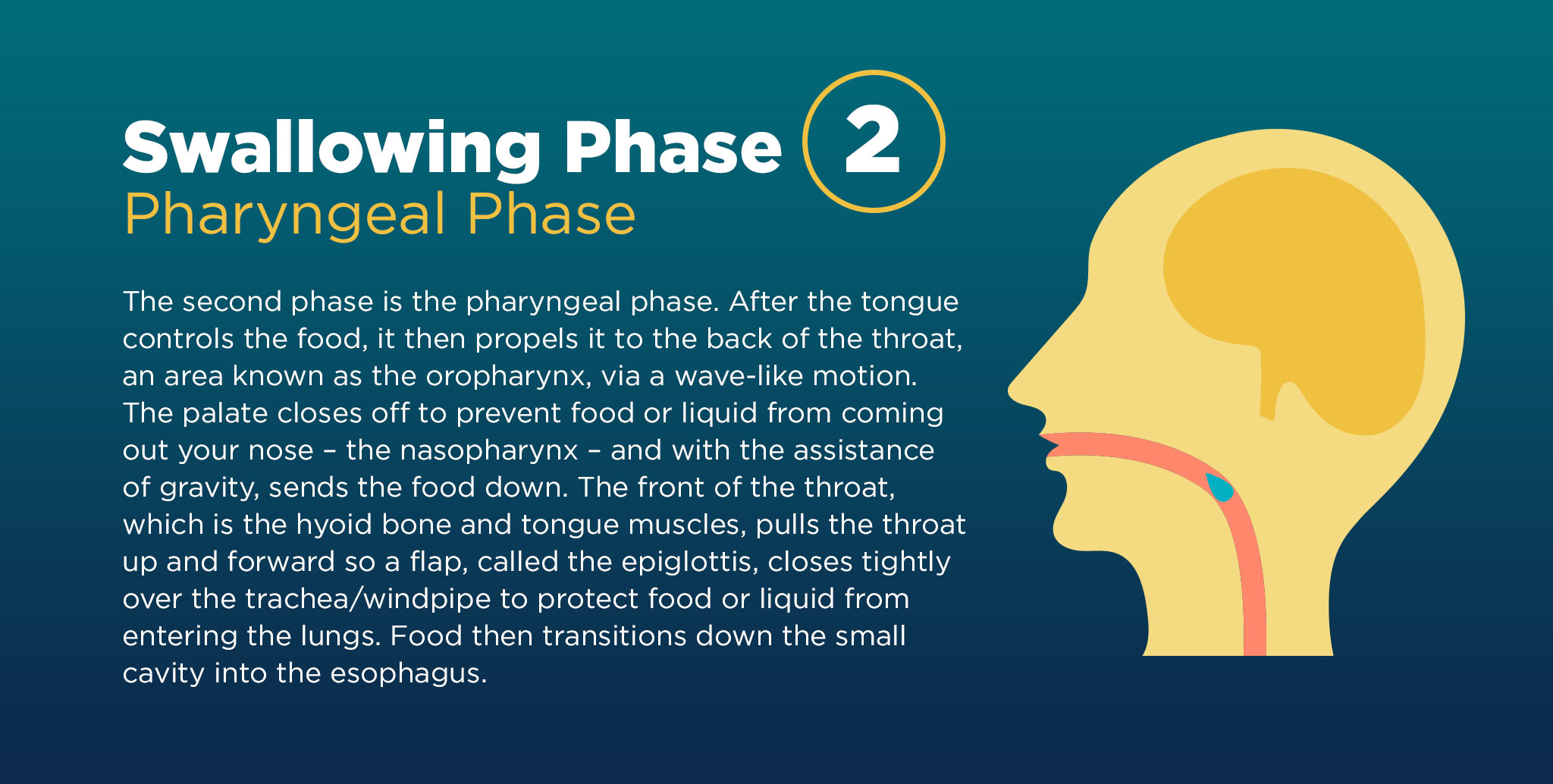
Phase Two: Pharyngeal Phase
The second phase for swallowing is the pharyngeal phase. After the tongue controls the food, it then propels it to the back of the throat, an area known as the oropharynx, via a wave-like motion. The palate closes off to prevent food or liquid from coming out your nose – the nasopharynx – and with the assistance of gravity, sends the food down. The front of the throat, which is the hyoid bone and tongue muscles, pulls the throat up and forward so a flap called the epiglottis closes tightly over the trachea/windpipe to protect food or liquid from entering the lungs. Food then transitions down the small cavity into the esophagus.
“It is during this phase when we may say, ‘Something went down the wrong pipe.’ Food or liquids could be going into the lungs, which is aspiration,” said Richardson. “Signs and symptoms of this are throat clearing, coughing, eyes watering and an uncomfortable painful sensation when swallowing.”
However, there are times when you can have food or liquids being aspirated and not aware of it. This is silent aspiration. If weakness in the oral phase is present, it can carry over to the pharyngeal phase and cause leftover residue or larger pieces of food to be stuck in the throat.
Phase Three: Esophageal Phase
Finally, the third phase in the swallowing process is the esophageal phase. This occurs when the top of the esophagus, the upper esophageal sphincter, opens, allowing the food to pass through, and then closes as the food continues traveling down to the stomach.

Testing for Swallowing Issues
When someone comes to see an SLP for a swallowing disorder, an evaluation is conducted to identify areas of dysfunction to treat in order to improve swallowing function and coordination.
If a bedside swallow exam cannot identify the deficits, then there are two additional options:
Modified Barium Swallow Study (MBSS) – an examination in which the patient would visit an outpatient hospital’s radiology department. The radiologist and the SLP will perform a swallow study using a white substance called barium. The barium will be a variety of textures and is viewed through x-ray to further determine the deficits and guide the clinicians to provide the best treatment plan.
Fiber optic endoscopic evaluation of swallowing (FEES) – a small scope is placed through the nasal cavity by the SLP to view the upper airway and throat. The SLP will view the breathing patterns and swallowing of saliva, and then use food and liquids occasionally, dyed green for contrast, to assess the function of the swallowing mechanism.
After the evaluation, an SLP will determine the best plan of care through swallowing exercises, biofeedback devices and/or neuromuscular electrical stimulation to rehabilitate the swallow function and keep each patient eating at the safest level possible.
Get the Help You Need at Brooks
Brooks Rehabilitation has certified SLPs at all levels of our system of care. Whether the patient needs an inpatient hospital setting, skilled nursing facility, outpatient clinic visits or home health, our highly knowledgeable and trained SLPs can help with most swallowing disorders.
Request more information or become a patient here.


