Brooks and UF researchers test novel combination of non-invasive stimulation and walking rehab for incomplete spinal cord injury
Back to physical health resource hub
Brooks Rehabilitation and University of Florida (UF) researchers have found that applying a non-invasive form of electrical stimulation to the lower spine during intensive walking rehabilitation was safe and feasible for people with chronic incomplete spinal cord injury, even those with considerable walking impairment. Results of the eight-participant clinical research study were published April 27 in the journal Spinal Cord.
Under the Brooks/UF-PHHP Research Collaboration, a formal partnership between Brooks Rehabilitation in Jacksonville and UF’s College of Public Health and Health Professions, the research team tested a novel combination of commercially-available transcutaneous spinal direct current stimulation, or tsDCS, to the spinal cord with simultaneous intensive walking rehabilitation to examine preliminary effects on walking function.
Principal Investigator Emily Fox, DPT, MHS, PhD, a research associate professor in UF’s department of physical therapy, clinical research scientist of the Brooks/UF-PHHP Research Collaboration and director of neuromuscular research at Brooks Rehabilitation led the research in collaboration with David Clark, ScD, a research scientist at the Malcom Randall VA Medical Center and associate professor in UF’s department of aging and geriatric research, and Kelly A. Hawkins, DPT, PhD, a research assistant professor of physical therapy at UF. Additional members of the Brooks study team included Louis DeMark, PT, DPT, NCS; Arian Vistamehr, PhD; Hannah Snyder, MS, ACSM-EP; Christy Conroy, PT, MSPT, NCS; Clayton Wauneka, PhD; and Geneva Tonuzi, MD.
All participants had a diagnosis of incomplete spinal cord injury, meaning they retained some motor or sensory function below the affected area; six of the eight participants had severe walking impairments and used a wheelchair for mobility.
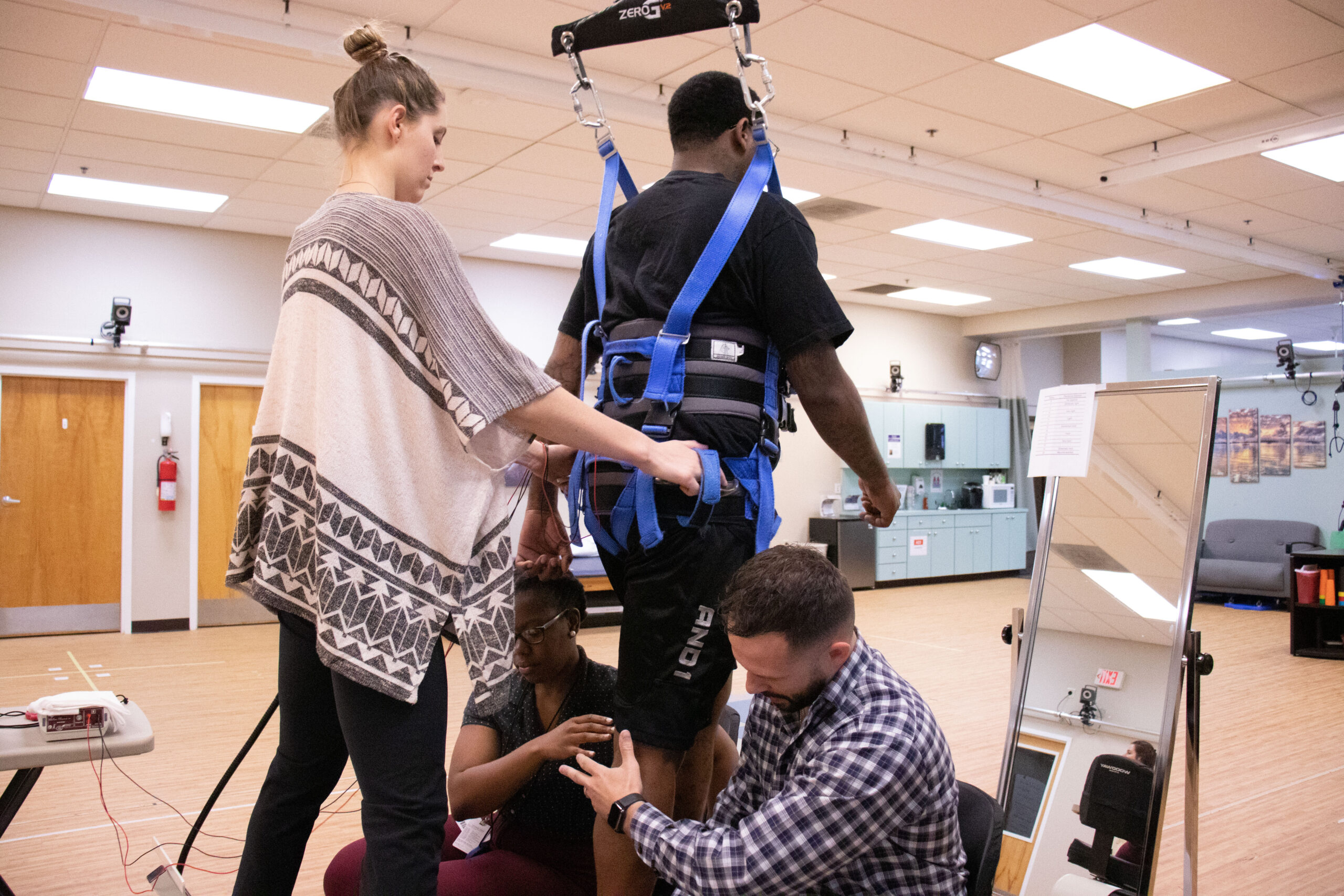
Half of the participants received tsDCS, while the other half received sham stimulation. (Similar to a placebo, a sham treatment is designed to resemble a real one to test efficacy.) All participants underwent simultaneous locomotor training, a form of task-specific walking rehabilitation.
The approach was tested over four weeks with four sessions a week. There were no major adverse responses to the treatments, the investigators reported. In addition, walking function was assessed with tests that were 10 meters in length and six minutes in duration. Gains in walking speed exceeded the benchmark for clinically significant difference in three of four who received tsDCS plus locomotor training and one of four who received sham stimulation plus locomotor training. Gains in walking endurance exceeded the benchmark in one of four in each group, the researchers reported.
“These combined techniques show promise as a beneficial rehabilitation approach,” said Dr. Fox. “Effective walking rehabilitation strategies are needed, and this approach can easily be used in a clinical setting, was well-tolerated by individuals with incomplete spinal cord injury and may have beneficial effects on walking function.”
“As a next step, the team will conduct a two-year study of the approach under a $400,000 grant by the Craig H. Neilsen Foundation. We will examine effects on walking function, including speed, endurance and quality, as well as investigate the effects of this treatment on spinal cord networks and how these networks function during walking,” said Dr. Fox.


