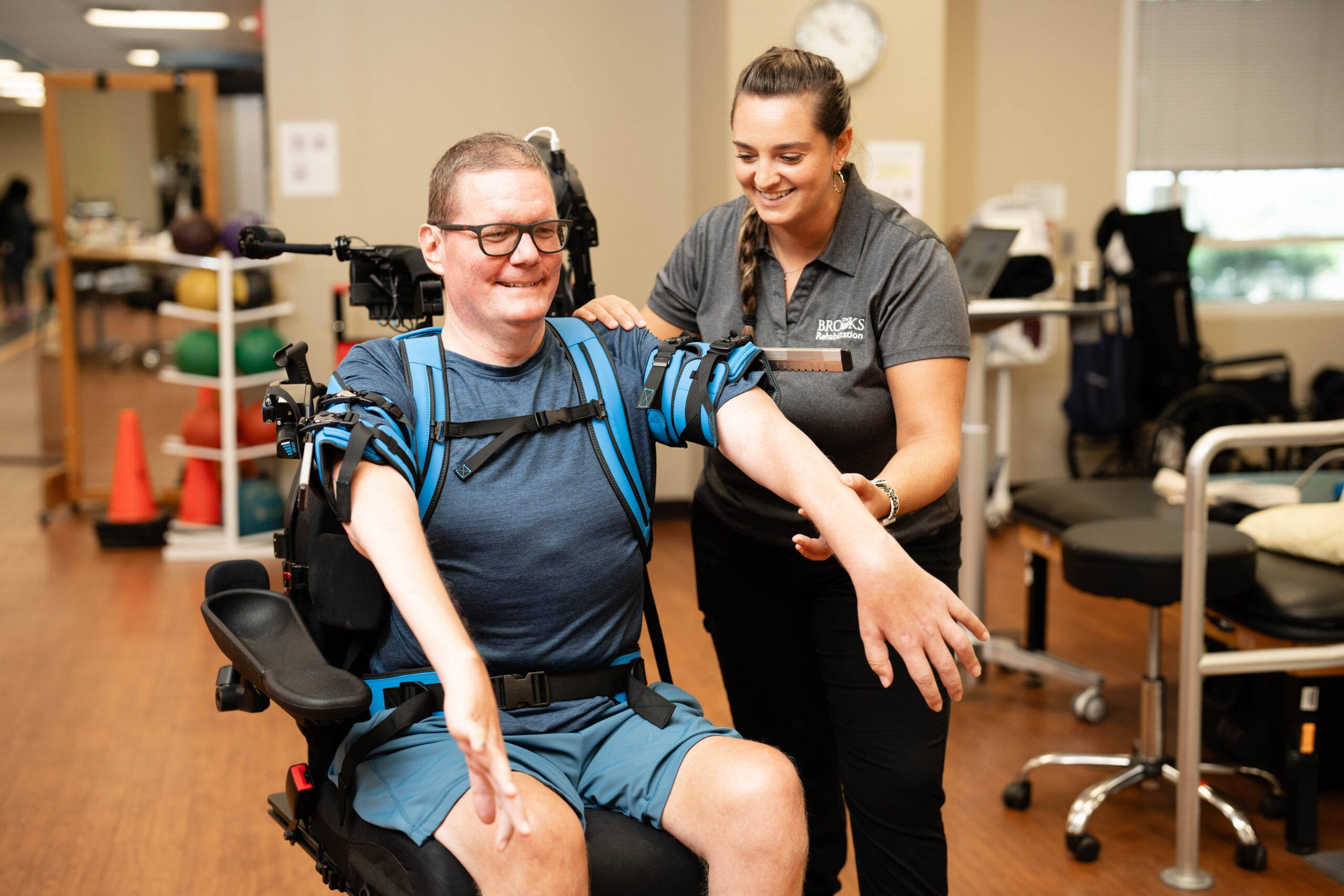
Our services
Need physical therapy, occupational therapy, speech therapy, cognitive or behavioral therapy? We have the right care setting with the right service to empower you to achieve your highest level of recovery.
Conditions we treat
As a leader in physical rehabilitation, we provide comprehensive rehabilitative services for multiple physical and neurological conditions for both adults and pediatric patients.
Get started at Brooks Rehabilitation
Latest News and Health Resources from Brooks
Education and guidance to support your recovery
From Silence to Strength: Chloe’s Inspiring Aphasia Recovery Journey
How a high school senior's determination and expert speech therapy helped her reclaim her voice after a life-changing diagnosis. One year ago, 17-year-old Chloe Karamsodkar was...